by Karen Keller Capuciati
I remember walking into Dad’s hospital room in Florida and seeing the deflated look on our mom’s face.
“What’s wrong, Mom?” I asked.
“They are testing Dad’s blood sugar now and have put him on a diabetic diet,” she said, with resignation. This was back in early 2006, during one of the multiple times Dad was hospitalized before he died in July of that year. There was already so much going wrong with Dad’s health, we just couldn’t bear the thought of adding diabetes to the list.
But that wasn’t the case. Dad’s doctor was merely monitoring his sugar (known as glucose) levels to prevent possible complications and create the best conditions for his recovery. Some illnesses, medications, and even trauma to the body — like surgery, for example — can cause blood sugar to rise. I can’t recall which of these applied to Dad on this particular hospital visit, but he had elevated blood sugar counts (the normal range is 70-110 milligrams per deciliter of blood), so his doctor was employing the same techniques he’d use in the case of diabetes, but only temporarily, to lower the glucose ratio in Dad’s body. There is usually a good reason for the monitoring and, in most cases, the practice is limited to the length of the hospital stay.
But this wasn’t completely communicated to us. We were told that his blood sugar was high, but not that there were special, short-term circumstances responsible for the elevated levels. So, naturally, alarms went off that this was a new, unexpected condition on top of everything else he was facing at the time. I’ve witnessed other similar events since then, with people’s reactions ranging from confused to downright irate about being given insulin in the hospital when they are not diabetic. It may have become common practice for today’s medical professionals, but to a patient it can be unnerving.
Patricia Capuciati Conwell, who happens to be my sister-in-law, has been an RN for 20-plus years and was the former director of the Diabetes Center at Backus Hospital in Norwich, CT. I asked her recently about this protocol, hoping she could clarify why even non-diabetic patients are having their blood sugar monitored these days. She explained that hospitals never really paid attention to glucose levels in the past, but it has become a mainstream practice in the last few years because medical professionals have found that close monitoring helps to cut down on a variety of complications.
“The two main complications that doctors want to avoid are infection and slowing down the healing process,” Patricia said. “Sugar feeds infection, and when the body is working harder to regulate the blood sugar, that impedes its ability to heal.”
“But there are so many factors involved,” she continued, “and a lot has to do with the reason the patient is in the hospital. For example, for heart surgery, they would want to keep the blood sugar tightly controlled to prevent infection, plaques from forming and blood pressure from rising — all to better facilitate healing.”
I asked Patricia about any side effects or concerns that come along with keeping strict blood sugar levels. After a thoughtful pause, Patricia responded, “The biggest one would be that your loved one’s blood sugar doesn’t drop too low. Find out what range the doctor is targeting and see how the patient feels.”
When blood sugars run high, insulin quickly brings it back down into a normal range. However, if it brings it down too far and the blood sugar dips below 70 mg/dL, this is called hypoglycemia. Lethargy, irritability, shakiness, sweating and confusion are some of the symptoms and side effects. You know those times when you feel a bit off and you realize it’s probably because you haven’t eaten all day? It’s essentially the same thing — your body doesn’t have enough fuel (glucose) to function properly. So, being that you know your loved one best, you are better able to identify if he or she is feeling crappy or acting out of the ordinary. In this case, let the doctor know.
“You might also talk to the doctor about a low-sugar, low-carbohydrate diet if it hasn’t already been ordered,” Patricia suggested as another way to help your loved one. “Why not have lots of vegetables and protein to keep the blood sugars down? This would also help the body’s natural insulin production and help maintain a more level range. Also, ask people not to bring up those chocolate milkshakes from the cafeteria or bring candy as gifts.”
Overall, Patricia stressed that communication with the medical team is key. Talk to the doctor to understand why they are monitoring your loved one’s glucose and what level they are trying to maintain, and ask about dietary adjustments. As always, be prepared, make a list of questions ahead of time, be an advocate for your parent and make sure you’re heard.
Karen Keller Capuciati is the Co-Founder of In Care of Dad.
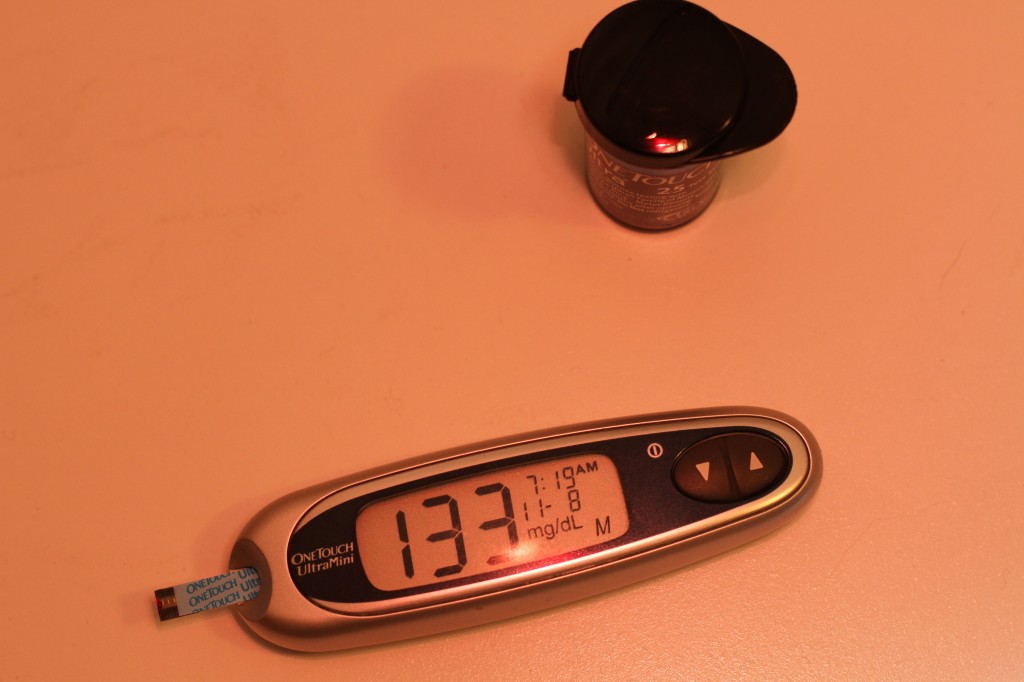
The photo was taken by Karen.






Interesting information, especially about the things that can affect blood sugar levels temporarily. My dad was diagnosed with brain cancer in 2010 and was put on very high levels of steroids in attempt to decrease swelling around the tumor. This treatment, we learned right away, can also cause high blood sugar. What we found most disturbing about that, though, was that some health care professionals seemed very concerned about those high readings and others, including his oncologist, said we didn’t need to worry about the levels at all and advised us not to bother with testing or treating for that. The back and forth of these differing opinions amongst the many doctors and nurses that were involved with his care was confusing and frustrating to us; we desperately wanted to be given one directive about the matter so we could be sure we were doing everything possible to care for him during the ten weeks he was so sick, before an infection (probably caused by the lowered immunity from the high dose steroids and the out-of-whack blood sugar levels). I agree with the point you made in your article: family members need to be provided with more – and more consistent – information!
I understand that it can be frustrating to a family when communications is not forthcoming from the doctors and nurses. Many time the nurse are simply doing what was ordered they are not privy to any more insight then the patients or their family are.
Another thing that can cause concern is when a patient is admitted on oral or no medication for diabetes and is switched over to insulin during their stay. This is another thing that is done routinely and not always well explained to the patient or family. This is done to maintain optimal blood sugar levels during the stay and sometime during the recovery period. When I was doing patient education I always stressed that the body has a higher demand for insulin during an illness / after trauma/ surgery etc because glucose levels typically rise during this time as the body attempts to heal itself. I also told the patients that just because they were on insulin during their hospital stay and recovery time didn’t mean that a year from now they would be but that sometimes the need for added insulin does not go away even after recovery.
It’s important to understood that diabetes is a progressive disease and that it isn’t uncommon for people to progress to the point of becoming insulin dependent over time even if they are doing everything right ( diet, exercise, medications, etc). Diabetes is a pandemic and projected to worsen in the coming years, so it is important to remember that treating in a precautionary way during a hospital stay is a good thing even if it does cause some anxiety. Another one of my patient lessons was to reinforce that when that doctor walks into your exam / hospital room they are your employee you are paying their wage in essence they work for you so don’t feel like you can’t ask them questions and make them explain them reasoning to you, after all they want what is best for the patient just like you do.